Introduction
Traditionally, gas permeable, scleral and even hybrid contact lenses are recommended for patients with keratoconus or other diseases that cause irregularity of the cornea, as they can effectively correct the significant levels of astigmatism through neutralization by the tear film. However, there is evidence to support the use of custom-made soft contact lenses designed for keratoconus in the management of this condition. These lenses are designed to conform to the irregular shape of the cornea while providing improved visual acuity (VA) and good comfort.
This case report presents the successful use of custom-made soft contact lenses in a patient with keratoconus, highlighting the benefits and potential advantages of this lens type in the management of this condition.
Subjective
This clinical account relates to a 27-year-old Caucasian male patient who was diagnosed with bilateral keratoconus. Following the diagnosis, the patient was recommended to start wearing contact lenses to reach better visual acuity. The patient was subsequently seen in our clinic approximately one-month post-diagnosis for the fitting of contact lenses.
Upon initial evaluation at our clinic, the patient reported experiencing a gradual decline in visual acuity over the past year, with worse visual acuity in his left eye. The patient also reported frequent itching in both eyes, which was accompanied by a habit of excessive eye rubbing. Despite the itchiness, the patient denied a history of hay fever or other allergic conditions, though they did report sensitivity to perfumes in soap-like products. The patient reported no significant medical history or current medication usage.
When evaluating a patient with a medical condition who is referred for contact lens management, it is our standard practice to gather information regarding their perceptions and expectations of contact lens wear in order to make an informed decision on the most appropriate lens type for the individual. During the consultation, the patient expressed concern regarding the potential discomfort associated with contact lens wear, specifically related to pain, increased itchiness, and stinging from solution.
Objective
| Spectacles (2021) | OD S-3.50=C-0.50×105 | OS S-2.75=C-0.25×178 |
| VA with specs | OD 0.9 | OS 0.6 |
| AR | OD S-3.50=C-0.75×74 | OS S-1.75=C-1.50×137 |
| VA with AR | OD 0.9 | OS 0.7 |
| Slit-lamp | Ectasia OS>OD, (-) striae, (-) Fleischer, (-) Munson sign | |
| Funduscopy | Healthy aspect OU | |
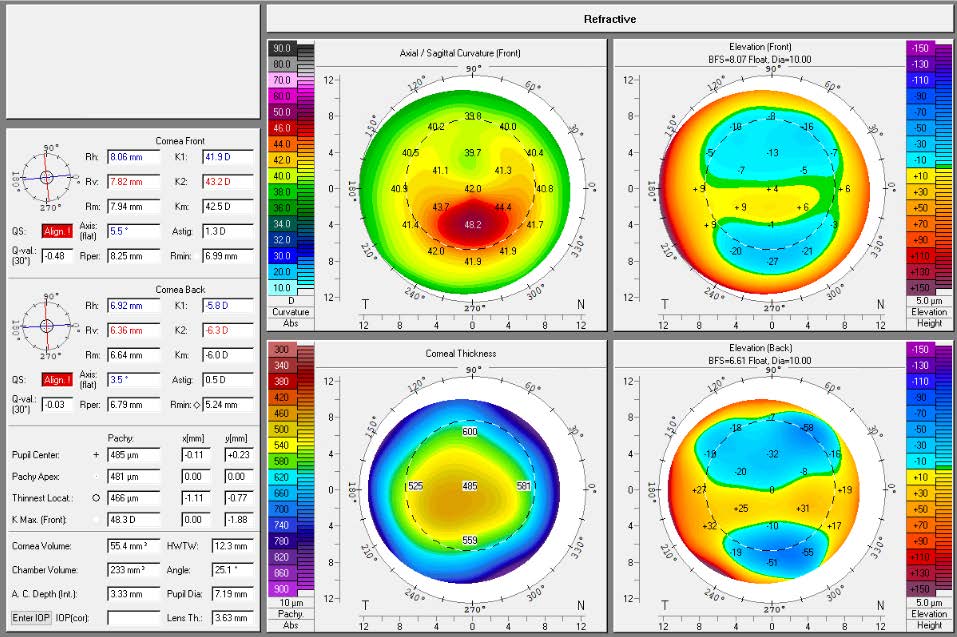
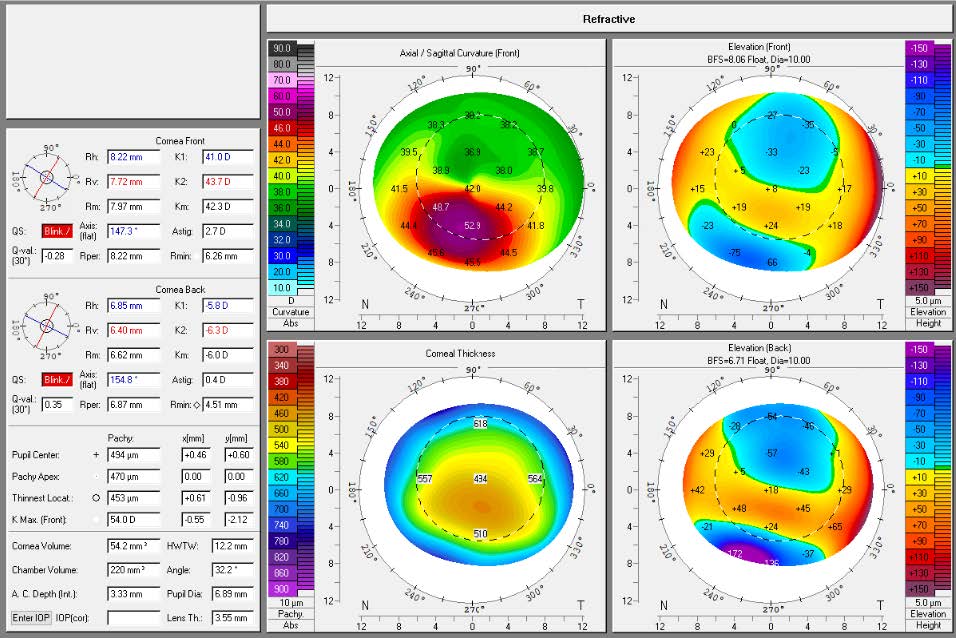
| Pentacam | ||
Assessment
Analysis of the collected data leads to the conclusion that the left eye experiences a greater level of visual deficit compared to the right eye. This observation is in agreement with the results obtained from a Pentacam tomographic analysis, which reveals steeper central K readings and a greater degree of corneal irregularity in the left eye. Although the left eye presents as more advanced compared to the right eye, both eyes are classified as stage 1 according to the Amsler-Krumeich grading system.
Considering that this patient expresses a negative attitude towards contact lenses, and rigid lenses may give firm discomfort in the beginning, this could result in a reluctance to wear contact lenses, despite improved vision compared to spectacles. To mitigate this, fitting the patient with soft contact lenses may be a more suitable solution.
In the past, fitting a keratoconic patient with soft contact lenses was not an efficacious strategy, as the soft lenses would conform to the irregular shape of the cornea. For this reason, vision correction with regular soft contact lenses did not yield an improvement beyond that achievable with spectacles. However, in the past years, there have been remarkable improvements in the design of soft contact lenses for treating keratoconus. These custom-made custom lenses are useful for correcting the early stages of keratoconus, for individuals with decentered cones, and for those who cannot tolerate rigid lenses.
The Kerasoft IC lens by Ultravision is one of the available lenses in this category. This design offers balanced overall thickness with spherical aberration control. It is advised to use a diagnostic fitting lens to evaluate the fit and determine the appropriate power of the lens. Following the fitting guide, the diagnostic lens with BCR 8.6 and a standard periphery was tried. Refraction was performed over the contact lens within 5 minutes of its insertion, yielding an over-refraction of OD S-3.25=C-1.00×45 & OS S-2.25=C-0.75×155, resulting in a corrected visual acuity of 1.2 OU, and 1.0 with OD and OS. The fit of the right lens was deemed adequate, while the left lens fit tightly at the edges. The laser mark on both lenses was correctly oriented.
Plan
The patient expressed a very positive reaction to the comfort of the contact lenses and was happy with the improvement of his visual acuity. He made the decision to commence wearing contact lenses. Hence the tight fit for the left eye and the over-refraction of the following contact lenses were prescribed for this patient:
OD Kerasoft IC / BCR 8.6 / S-3.25=C-1.00×45 / periphery standard / diam. 14.5
OS Kerasoft IC / BCR 8.6 / S-2.25=C-0.75×155 / periphery flat 1 / diam. 14.5
In Summary
Custom-made soft contact lenses with a special design can be helpful for people with keratoconus and provide a unique solution for those with irregular cornea shapes. The VA with these lenses is better than with spectacles in contradiction to the VA with regular soft contact lenses. These contact lenses should be considered as a way to manage keratoconus for individuals with early stages of keratoconus or decentered cones, and for those who cannot tolerate rigid lenses.
This case study is part of a series focusing on speciality soft lens fitting. Stay tuned for the next installment coming soon. Special thanks to Eef van der Worp for bringing this series together.